One evening several years ago, MiKaela Olsen, D.N.P., sat on her porch with a neighbor and spoke firmly and frankly to her as both a friend and a professional. Olsen, a Johns Hopkins Kimmel Cancer Center clinical nurse specialist, was concerned. The neighbor, a mother of two young children, had breast cancer and was strongly considering foregoing chemotherapy to avoid losing her hair — despite the fact that adding chemotherapy to surgery and radiation would reduce her risk of disease recurrence by about 90%. Choosing not to get chemotherapy would increase her risk of recurrence by at least 30%. Olsen eventually persuaded her friend that bypassing chemotherapy was not worth the increased risk to her long-term health.
Olsen’s neighbor is not the only breast cancer patient who needed convincing. Many anti-cancer drugs work by killing rapidly dividing cells. Normal cells like hair cells that also divide rapidly are collateral damage. For decades, the bald head has been the iconic symbol of cancer therapy, an outward and visible sign that immediately identifies a person as a cancer patient. According to recent research, 47% of female cancer patients deem hair loss the most traumatic aspect of chemotherapy, and 8% of patients say they would decline chemotherapy to avoid losing their hair.
“I don’t want anyone to make a decision about whether or not to have chemotherapy based on the risk of hair loss,” says Olsen, who is excited about a new product that may eliminate or at least diminish this dreaded hallmark of cancer treatment.
Starting this fall, Kimmel Cancer Center patients with breast and gynecologic cancers will have the option to use a new device that prevents or minimizes chemotherapy-induced hair loss. The use of the device will be quickly expanded to patients with other tumor types.
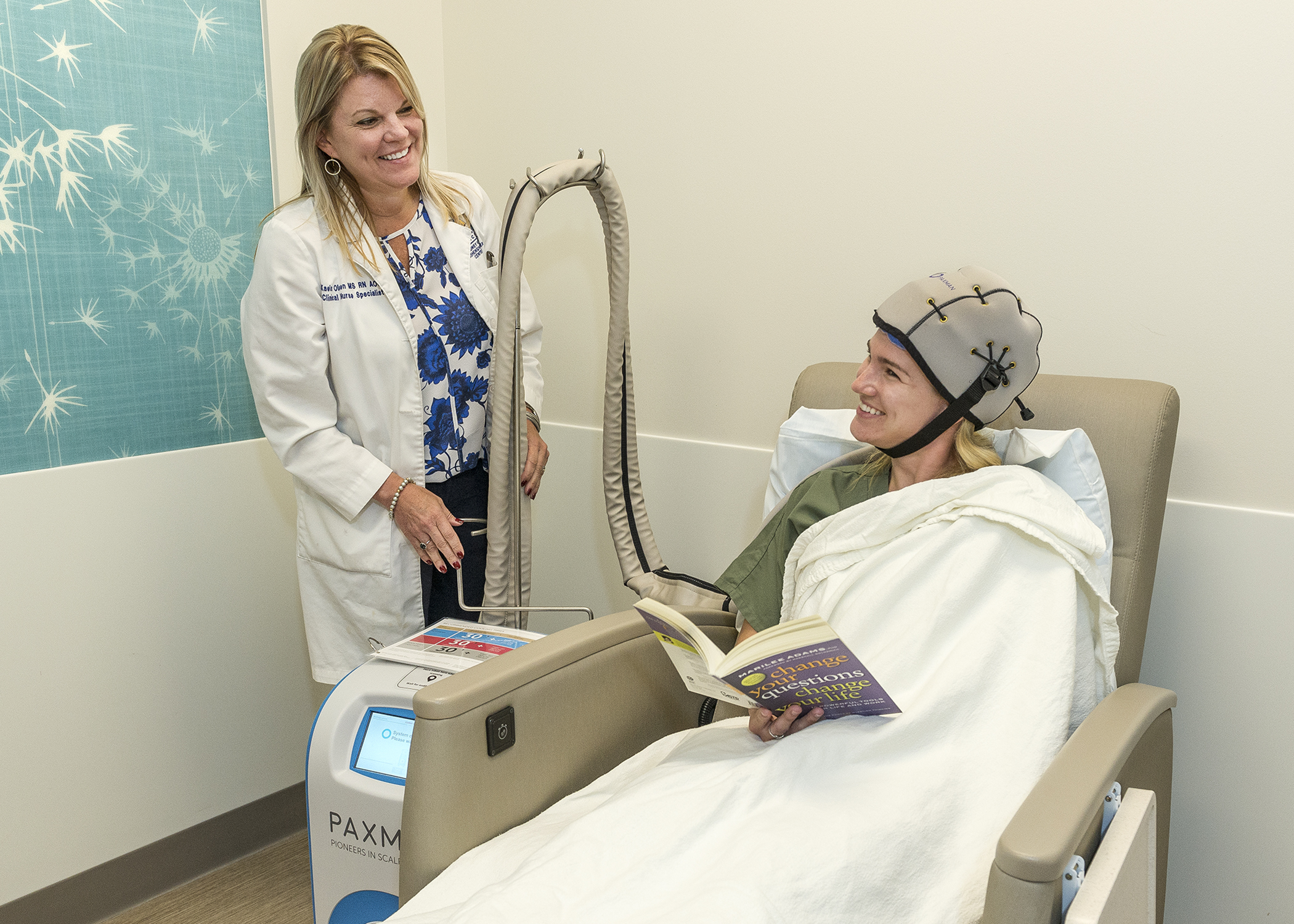
The Paxman scalp cooler, also known as a “cooling cap,” works by reducing the amount of chemotherapy that reaches hair follicles. Patients wear the cap on their head during chemotherapy infusions and for a brief time before and after chemotherapy. The cap, which is attached to a compact and mobile refrigeration system, evenly cools the scalp as blood vessels constrict, reducing blood flow and ultimately lowering the amount of the chemotherapy drug that gets to hair follicles. Patients feel the chill, but the cold cap doesn’t cause pain.
The scalp cooler is the only device approved by the Food and Drug Administration that is proved to minimize hair loss in patients undergoing chemotherapy. It works best for patients receiving a class of drugs called taxanes. In one study of more than 5,000 patients, over 70% of those receiving taxane-based chemotherapy did not lose their hair.
The Kimmel Cancer Center is one of only a few cancer centers in Maryland offering cooling caps to patients. The cost varies depending on the number of times a patient uses the cap, but it can go as high as a few thousand dollars. It is not covered by health insurance, but financial assistance is available to patients in need. Vered Stearns, M.D., Director of the Women’s Malignancies Program, is working to identify funding partners to make the cooling caps accessible to all patients.
To learn more about how you can support making cooling caps accessible to all patients, please contact the Johns Hopkins Kimmel Cancer Center Development Office:
Elizabeth Raymond, Sr. Associate Director of Development
750 East Pratt Street, 17th Floor, Baltimore, MD 21202
Tel: 410-361-6183
Email: [email protected]